Spinal Disc Health: Why the Right Recovery Plan Matters After a Back Injury
If you've ever been told to "just strengthen your core" after a back injury, you've experienced one of the biggest problems in spine care: generic advice for a deeply individual problem.
The truth is, your spinal discs follow a strict set of rules — and those rules change the moment an injury occurs. Understanding what's happening inside your spine is the first step toward a recovery plan that actually works for your body, not someone else's.
At Chicago Spine + Sports, we treat spine and disc issues every day, from weekend warriors in Lincoln Park to competitive athletes across the city. Here's what we want every patient to know about how disc health really works.
Your Spine Needs Stress — Until It Doesn't
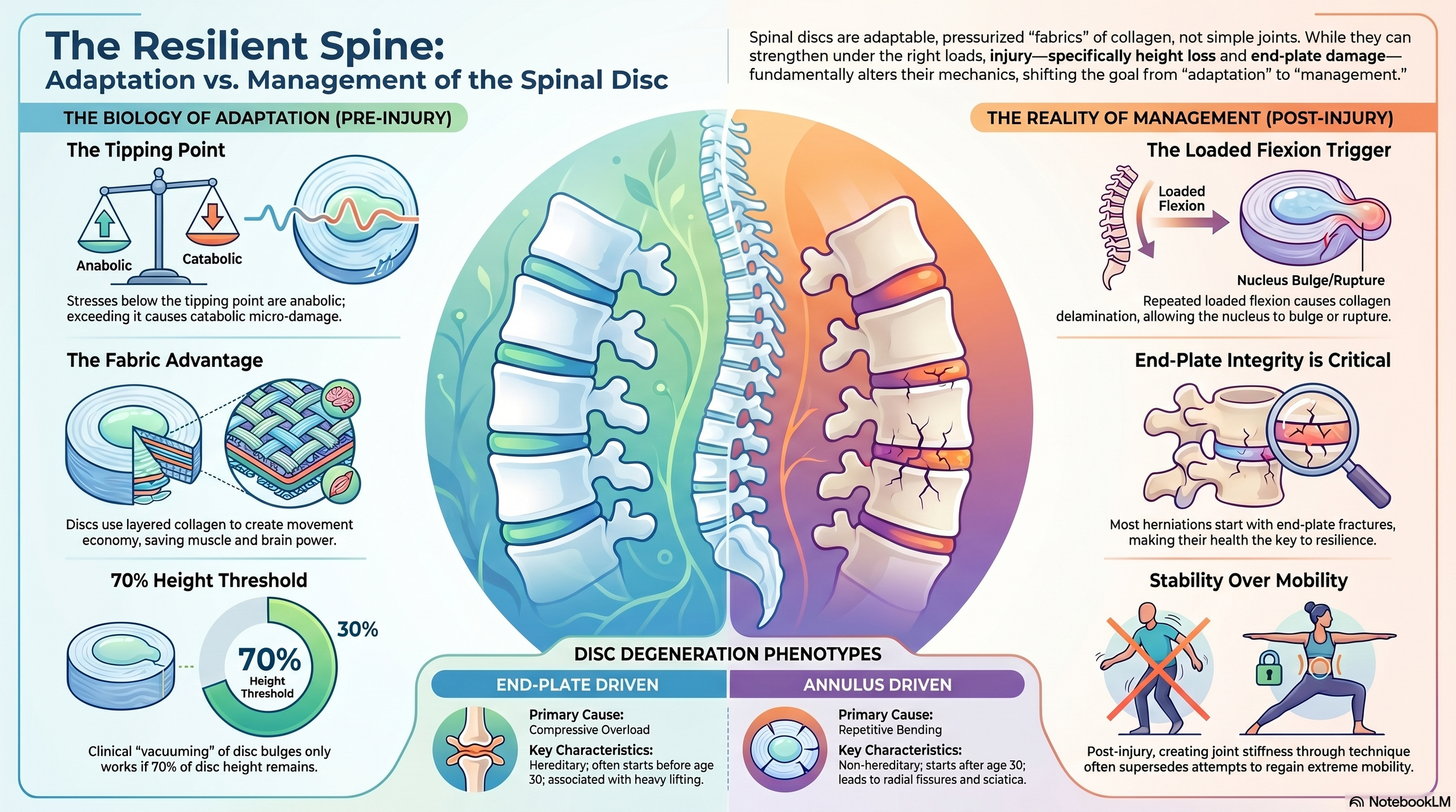
Every tissue in your body adapts to the loads you place on it. Bones get denser. Muscles grow. And yes, your spinal discs become more resilient when challenged appropriately.
But there's a tipping point.
When mechanical stress stays below that threshold, your body builds itself stronger (an anabolic response). Push past it, and the same stress starts breaking tissue down faster than it can repair (a catabolic response). Micro-damage piles up. Eventually, you have an injury.
Where exactly that line sits is different for every person. Genetics, training history, body type, age, and prior injuries all shift the equation. This is why two people doing the same workout can walk away with completely different results — one feeling stronger, the other in pain.
The Trade-Off Most People Don't Know About
Spinal discs face a unique design challenge: they can't be optimized for both extreme mobility and heavy load-bearing at the same time.
Mobility-focused training (think yoga, gymnastics) softens the binding collagen in the disc, allowing greater range of motion but reducing stiffness.
Load-focused training (think powerlifting, football) stiffens the collagen and strengthens the bony end plates to handle compression — but limits flexibility.
That's why a powerlifter and a yogi have fundamentally different spines, even before you factor in injury history. Neither approach is wrong — but training one way and demanding performance the other way is a recipe for breakdown.
What Actually Happens When a Disc Gets Injured
Here's something most people aren't told: roughly 65% of disc herniations are preceded by a fracture in the vertebral end plate — the thin layer of bone that caps each disc.
When the end plate fails, two things happen:
Disc height is permanently lost. The hydraulic, gel-like nucleus inside the disc loses its ability to dissipate stress evenly. Imagine the difference between a fully inflated tire and a flat one — same structure, completely different mechanics.
The degenerative cascade begins. With less disc height, your facet joints take on more load than they're designed for. Inflammation can become chronic, especially when fragments of bone interfere with your body's natural healing response (this is what shows up on MRI as "Modic changes").
The unfortunate reality is that many of these changes are not reversible. This isn't meant to scare you — it's meant to underscore why early, personalized intervention is critical and why one-size-fits-all rehab protocols often fall short.
Your Body Type Changes Your Risk Profile
Modern spine care is moving toward what physicians call "precision medicine" — treating the individual in front of you rather than a textbook average. When it comes to disc injuries, body type plays a major role.
Slender, lean-framed individuals (think distance runners, golfers) tend to have ovoid-shaped discs. Their spines are more flexible and twist easily, but stress gets distributed diffusely and they're less resistant to buckling under heavy load.
Heavier, broader-framed individuals (think linemen, throwers) tend to have lima-bean-shaped discs that concentrate stress in the back-and-side regions. They handle compression beautifully but can fracture if forced into deep bending.
Posture matters too. Patients with flat backs (hypolordosis) often feel fine standing but accumulate flexion stress when sitting — a major risk factor for posterior disc bulges. Those with deeply arched backs (hyperlordosis) often feel the opposite: tight when standing, relieved when seated.
Knowing where you fit on this spectrum changes everything about how we'd program your rehab or training.
Popular Exercises Are Not Universally Safe
A perfect example of why context matters: the Jefferson Curl — a segmental spinal flexion exercise that's gone viral in fitness circles.
For a healthy athlete looking to develop neuromuscular control of the deep spinal stabilizers, the Jefferson Curl can be a useful tool. But for someone with existing disc height loss or shear-triggered pain, it's often exactly the wrong choice. When the spine is fully flexed, the erector spinae muscles flatten out and lose their angled support structure, transferring shear load directly to the disc.
The same principle applies to the McKenzie press-up (the "floppy push-up"). It can genuinely help draw a disc bulge back into place — if at least 70% of disc height remains. But used for too long, it over-sensitizes the facet joints and creates a new pain pattern.
The lesson: there are no universally good or bad exercises. There are only exercises that match — or don't match — your specific situation.
What Recovery Actually Looks Like
After a real disc injury, the goal of treatment shifts. We're no longer trying to "rebuild" the disc to its pre-injury state — that's not biologically realistic for most patients. Instead, effective rehab focuses on:
Stabilization — using muscle co-activation to replace lost joint stiffness
Desensitization — identifying which movements trigger pain and which don't, so you can move confidently again
Pain reframing — treating pain as useful information about what your spine needs, not an enemy to push through
Done right, this approach gets people back to running, lifting, golfing, chasing their dogs around the lakefront — whatever they love — without the constant fear of re-injury.
Why Programming Is the Most Important Decision You'll Make
Here's the bottom line: whoever designs your rehab program — your physical therapist, your chiropractor, your strength coach — has more influence over your long-term spine health than almost anyone else in your life.
If they're working from a generic protocol, you're getting generic results. If they're matching the program to your phenotype, your injury history, your goals, and the specific mechanics that trigger your pain, the outcomes look completely different.
That's the standard of care we hold ourselves to at Chicago Spine + Sports. Every patient receives a comprehensive movement assessment before we prescribe any exercise. We identify your specific pain triggers, map out the mechanical patterns driving the issue, and build a plan that fits you.
Ready to Get Your Spine Assessed?
If you're dealing with persistent back pain, a recent disc injury, or you just want to train smarter and avoid future problems, we'd love to help.
We work with athletes, lifters, runners, weekend warriors, and everyday Chicagoans who want their spines to last as long as they do.
Chicago Spine + Sports is a chiropractic and sports rehabilitation clinic serving the greater Chicago area. Our team specializes in evidence-based, individualized care for spine and sports injuries.